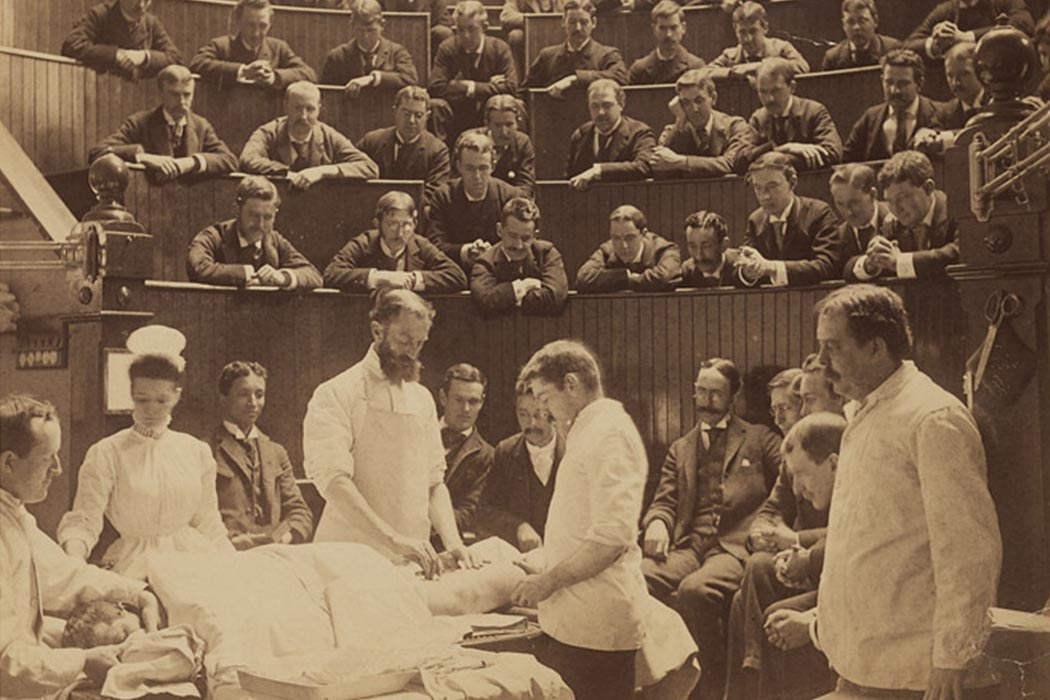
Director Steven Soderbergh’s historical drama series, The Knick, brings viewers inside a New York City hospital’s operating room in the year 1900. In last year’s series premiere, an anesthetized pregnant woman, diagnosed with placenta previa, a condition in which the placenta covers the opening of the cervix, lay vulnerable on the table. At the turn of the 20th century, previa was a major concern, as women with this condition often bled out during delivery. The Knickerbocker’s chief of surgery, Dr. J. M. Christiansen, had been experimenting with a preventive measure, and this was his twelfth stab at it. He turned to the more than three-dozen spectators filling the tiered wooden benches that surround the surgical stage, gave a rousing speech, and pledged to finish in “100 seconds.” Time, he believed, was more important than technique.
Once he slices her underbelly and the blood begins to gush, however, his audience—both those in the room and we at home—realizes that success still eludes the surgeon. The scene is ghastly to watch, and yet, we do. We also post and pin gruesome pictures from digital collections of historical medical images; gaze at exhibits of pathological waxworks; tune in to televised live brain surgery; and read books like Richard Barnett’s The Sick Rose: Disease and the Art of Medical Illustration (2014) and his recent follow-up, Crucial Interventions: An Illustrated Treatise on the Principles & Practice of Nineteenth-Century Surgery (2015). One might conclude that we are having a moment with the morbid.
But this type of voyeurism is hardly new, and the surgical theater is one of the more glaring examples. It was born of the anatomical amphitheaters of the Renaissance, where public dissections were held a few times per year to expose the “secrets of Nature revealed by God.” For the price of admission, one could watch as doctors performed an autopsy on the body of a convict. As Julie V. Hansen describes, “In the anatomical theater, which was lit by scented candles to augment the dim light drawn from windows and sometimes featured music played by a flutist…they took on a festive and theatrical atmosphere.” The use of the words theater and theatrical is entirely appropriate; the dissections were a form of entertainment.
The similarity between the grisly anatomical theater and the burgeoning surgical theater of the early 19th century is such that, Barnett writes in Crucial Interventions, even the Renaissance-era anatomist Hieronymus Fabricius (1537–1619), known as the father of embryology, would not have felt out of place in the “modern” space. “Well into the 1840s, Fabricius would have recognized much of what went on in those noisy, dirty, crowded spaces called operating theaters.”
Surgical spaces were indeed noisy, dirty, and crowded throughout much of the 19th century. The racket could be largely attributed to the screaming and wailing of patients. Until the widespread use of anesthesia in the second half of the century, all procedures, including amputations, took place while the patient was wide awake, perhaps slightly eased by some bad liquor. Nitrous oxide (laughing gas) was determined to be an effective painkiller earlier in the century, but it was not widely employed to subdue the sick. Ether was another substance with acknowledged anesthetic potential, but it wasn’t until 1846 that an enterprising dentist convinced Dr. John Collins Warren to attempt a surgical trial. After that success, patients began to demand palliatives, and most doctors found themselves able to undertake more surgeries and with improved dexterity.
Although anesthesia made for a quieter operating theater, it didn’t substantially lower rates of postsurgical infection. As Barnett describes in Crucial Interventions, the surgical room itself—not to mention the doctors’ bare hands and street clothes—was crawling with harmful bacteria and microorganisms. Louis Pasteur had issued his laboratory findings about the germ theory in the 1860s and ’70s, but acceptance among physicians was slow. Some, like Joseph Lister (1827–1912), made the first step in antisepsis by applying carbolic acid directly to wounds. William Stewart Halsted (1852–1922), incidentally the man on whom The Knick’s star surgeon, John Thackery, is loosely based, made his contribution to surgical hygiene by contriving rubber gloves. That was just a happy accident, however; the gloves had been designed to minimize the effect of harsh antiseptics on the nurses’ hands.
Both before and for a few decades after the germ theory was on the table, operating theaters were congested places where, writes Barnett, “a crowd of spectators witnessed dramatic triumphs and tragedies.” In 1887, Dr. Lawson Tait recalled a time 25 years earlier when “every seat even of the top gallery was occupied. There were probably seven or eight hundred spectators, for Syme was to operate on a gluteal aneurysm.…The older and more experienced spectators went mostly from curiosity, and perhaps to be able to say that they had seen the great surgeon do this great deed.”
Some surgeons were indeed a draw, and they seemed to revel in the showmanship aspect of their work. Scottish surgeon Robert Liston (1794–1847) “operated with a knife gripped between his teeth,” writes Barnett. Working largely without anesthesia, Liston was celebrated for his quick and dirty amputations. Tait was not impressed, writing of Liston, “he made a reputation, and leaves a memory more like that of an actor than a man of science, as he really was.”
The language used to describe surgical theaters supported this idea that surgery was a performance, with drama, gore, nudity, and death just part of the act. For example, the operating theater of Jefferson Medical College in Philadelphia was commonly known as the “Pit,” as in the area where orchestra musicians perform. Other operating theaters were likened to circuses and magic shows. In her 2014 book, Dr. Mütter’s Marvels, Cristin O’Keefe Aptowicz reports that charismatic Philadelphia surgeon Thomas Dent Mütter (1811–1859) was compared to P. T. Barnum. It was meant as a compliment. Writing in 1900, Dr. Frederick Treves described an early 19th-century surgeon in this manner: “He stepped into the arena of the operating theater as a matador strides into the ring. Around him was a gaping audience and before him a conscious victim, quivering, terror-stricken, and palsied with expectation.” The applause a surgeon received upon entering the theater only heightened the spectacle, complete with rows of ogling observers.
But who were all these onlookers? Chiefly, they were professors of medicine and medical students. As the medical establishment moved away from Galenesque ideas of illness as an imbalance of humors, toward a scientific, anatomy-based approach, operative practice gained traction, and that required specific knowledge and training. Family members also were allowed inside the operating theater, writes Gordon Hendricks, whose research into Thomas Eakins’s The Gross Clinic painting states that next of kin not only were admitted to the inner sanctum but also required by law in charity cases; in the 1875 painting, a woman thought to be the patient’s mother sits just behind the doctor, covering her eyes. And while on the subject of Eakins, his portrayal of the Jefferson Medical College’s operating theater includes the surgeon’s son and “Hughie,” the hospital’s janitor, as interested bystanders. On The Knick, even hospital administrators occasionally sit in on operations, and, in one memorable episode, an armed gangster was permitted to watch the surgeons attempt to save his henchman’s leg, while he threatened them from the stands. (The Cinemax series strives for historical accuracy, and its consultant, Dr. Stanley Burns, said in a recent interview that the scene was entirely plausible.)
It’s worth noting that when Eakins created another operating theater painting in 1889, this one called The Agnew Clinic, it again depicted an overcrowded chamber of attendees peering down on the godly surgeons. (The Agnew Clinic was exhibited at the 1893 World’s Columbian Exposition in Chicago, arguably generating an additional audience for the surgical act—fairgoers.) The Burns Archive, a collection of more than 1 million historic photographs curated by Burns, contains a stunning photo of a Philadelphia operating theater in 1902 with so many rows full of viewers, it would put most community theaters to shame. Burns said he believes the attraction, especially at the turn of the century, was the chance to witness medical miracles. “Of course it had a spectacle aspect, because you were watching innovation,” he said. “It was a performance just like someone dancing on a stage.”
By 1917 old-fashioned operating theaters had become obsolete for several reasons. One, said Barnett in a recent interview, was the competent use of anesthetics. “Once you don’t have a bawling patient, it’s no longer as big a spectacle.” Two, as surgeons began to realize that speed wasn’t the variable that was causing disastrous results—that indeed slower, meticulous incisions proved more efficacious—there was altogether less drama associated with the surgical stage. The absence of a ticking clock and of a surgeon bellowing, “Time me!” spoiled some of the excitement.
The primary explanation for the demise of the antiquated operating theater, however, was the acceptance of asepsis. The idea that spectators, especially fellow doctors direct from postmortem examinations, might carry germs into the surgical space was not unanimously agreed upon, even into the Gilded Age. Those who believed in germ transfer went so far as to devise special operating tables shaped to prevent “spectators crowding over the operator’s shoulder.” Others mimicked theaters seen in Europe by installing a glass screen “hermetic in its imperviousness…interposed between the onlookers and the operator and his assistants.” Dr. W. J. Smyly modernized his theater with a screen in 1897 in order to mitigate dust, drafts, and “germs floating in the air” as a precautionary measure. “I do not want to attach too much importance to the purity of the atmosphere, but I cannot regard it as altogether unimportant, and experiments have proved that it is not so.”
Once a Week
“What really drives [operating theaters] out of existence is germ theory,” said Barnett, “and the realization that these big, crowded theaters are extremely unhygienic.” When doctors and surgeons finally accepted the fact that more bodies in the room meant a greater possibility of infection for the patient, tighter control was exerted on the operating space. These controls included better lighting, steel or glass worktables, easy-to-clean tile floors, and very little room for bystanders. Coincidentally, many hospitals were undergoing renovations and rebuilds at the turn of the century (the Knickerbocker among them, in season two of The Knick, airing now). “The rise [in the volume of ] surgery marked a major change in hospital architecture,” writes Annmarie Adams in “Modernism and Medicine,” causing “the transformation of the old-fashioned operating theater into the operating suite.” And the modern, secluded, scientific operating suite was, writes Thomas Schlich, “decidedly not a public space.”
The age of the surgeon showman was over—but that doesn’t mean our desire to mingle with the macabre has waned. “To this day, people are fascinated by these procedures,” said Burns, who offered as an example the fact that some hospitals offer video monitors to watch a surgery in progress. Burns also is involved with a new medical drama, Mercy Street, which is set in a field hospital during the Civil War and will premiere on PBS in January. We’ll be huddled around our screens in anticipation.