Could yellow fever be the next Zika? With warnings that a shortage of the vaccine against the virus could spur on a new epidemic, yellow fever is again in the scientific spotlight. Modern responses to yellow fever tell a story of globalization and scientific progress. But the responses of the past tell, in part, the story of women. Randall L. Hall explores gender and race relations in the 19th century South through an 1878 yellow fever epidemic in Memphis.
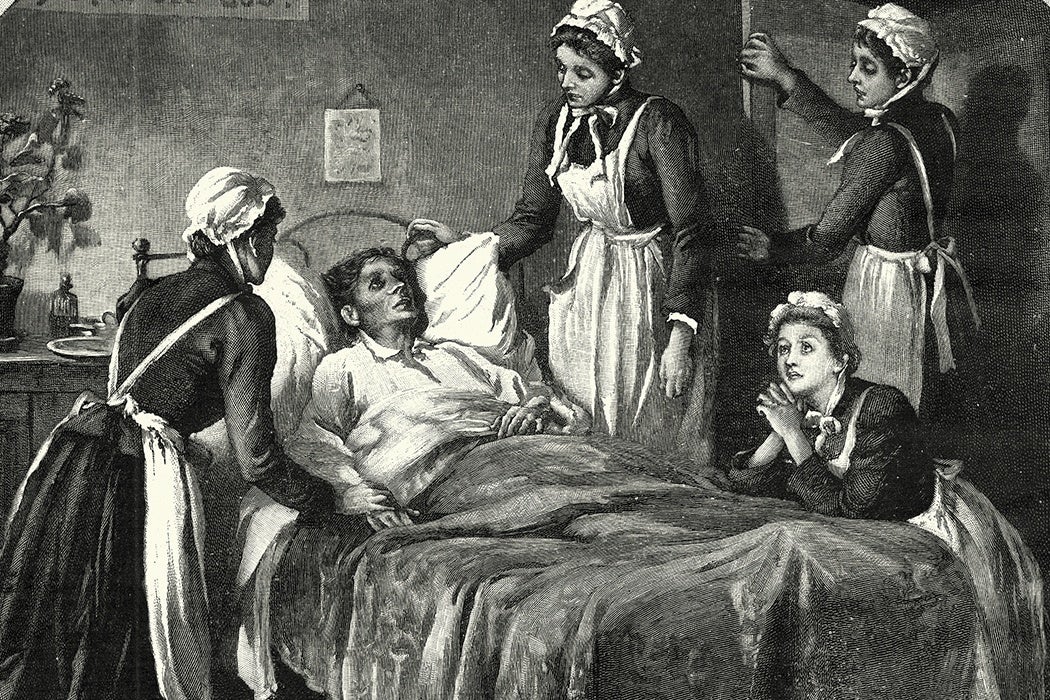
At the time, writes Hall, women who nursed were seen in dramatically different lights. Nuns from Memphis’ Catholic and Episcopal orders were painted as religious heroines, but other nurses were dismissed and vilified for challenging the “proper” roles of women. Hall tracks the stories of Kezia Payne de Pelchin and E. Kate Heckle, two Texas transplants who came to Memphis to nurse the sick. They were not welcomed with open arms—rather, they faced what Hall calls “the prejudice and scorn of a southern society that believed firmly in a restrictive definition of woman’s proper place.”
These prejudices were already reflected in the fact that, despite nursing advances during the mid-19th century and the rise of professional nursing elsewhere, Southern nursing was not professionalized at the time.
Despite those prejudices, nearly 3,000 women worked as nurses on yellow fever’s front lines. Women from out of town were only paid $4 per day; women from within Memphis and black women were paid $3. In contrast, doctors were paid $60 per week. They were treated as social inferiors and refused accommodation at the city’s finest hotel, which put up doctors. Gender conflicts prevailed in the sickroom, too, and arguments broke out over things like treatment duties and breaks.
Class and cultural tensions prevailed, but Hall writes that racial tensions were at the heart of the worst discrimination faced by nurses. Black nurses were assigned the most uncooperative patients and faced daily struggles over duties, responsibilities, and competency.
Despite their heroic efforts of nurses of all races, 20,000 people died of yellow fever in the Mississippi Valley during the epidemic—over 5,000 of them in Memphis. Even that terrifying crisis was not enough to overcome prevailing racial, class, and gender tensions, Hall writes. Who knows what tensions a 21st-century epidemic might expose?