Dogs have long been known for their incredible sense of smell. As the earliest domesticated animals, they have also developed unique skills for working closely with humans and reading our social cues. Together, these traits allow them to excel at detecting, locating, and alerting humans to volatile compounds–or, in other words, scents. In some fields, dogs are considered the “gold standard” for identifying and distinguishing target scents across a variety of contexts. We encounter these kinds of working dogs all the time, on search and rescue teams, bomb squads, drug enforcement agencies, and even conservation projects. Scent detection dogs in these fields regularly feature as heroes alongside their human counterparts in books, movies, and news articles. As these stories portray, there is likely no greater feeling than the touch of a cold canine nose when one is buried in an avalanche or the rubble of a collapsed building.
Behind the scenes, scent detection dogs have also been able to accurately detect infection, including C. difficile (a bacterial infection often acquired in healthcare settings) and malaria, in both human patients and biological samples. They can also identify many types of cancer, including (but likely not limited to) skin, lung, breast, and bladder cancers. For example, one study tested dogs for the detection of both lung and breast cancer in breath samples collected from patients. Following a 2-3 week training program, the five dogs were able to distinguish positive lung cancer samples from negative samples 99% of the time, and positive breast cancer samples from negative samples 88-98% of the time. Interestingly, each of the dogs included in this study were household dogs with only a basic obedience class and the drive to work in their toolkit. As this example illustrates, trained animals have similar–or in some cases, higher–success rates than medical devices and laboratory procedures.
Weekly Newsletter
Dogs can work through many samples quickly, at a low cost, with minimal or no interaction with patients. For example, healthcare workers can collect breath, sweat, urine, or blood samples for dogs to process, rather than having the dog examine patients directly. This allows the dogs to work with minimal environmental distraction, and bypasses the necessity to work directly with patients who may be uncomfortable around dogs. Despite these advantages, the chances are low that your routine blood draw or breast biopsy is being examined by a dog in the laboratory. For now, the only dogs you’ll meet in the hospital hallway are mood-boosting therapy dogs, and service dogs aiding their handlers (also both worthy canine causes).
As we enter the third year of the COVID-19 pandemic, with no clear or simple end in sight, biomedical scent detection dogs in the healthcare industry seem to have a lot to offer. Surges in the virus overwhelm COVID testing sites and strain hospitals, with rapid spread and cases of severe illness. In addition to the direct effects of the pandemic, intense demands on healthcare systems around the world have reduced our ability to maintain control of the spread of other viruses such as malaria and HIV, disrupt preventative or routine care, and delay surgeries for chronic conditions. Countries will likely face backlogs on healthcare demands for years to come, even when the pandemic is under control. Utilizing dogs in healthcare settings has the potential to help us get caught up with these delayed procedures such as cancer screenings.
In addition, and more to the point, there is evidence that dogs can quickly and accurately detect COVID-19 infection. “Scientists […] suggest that canines could help to control the pandemic because they can screen hundreds of people an hour in busy places such as airports or sports stadiums, and are cheaper to run than conventional testing methods […]” notes science journalist Holly Else in Nature NEWS. While PCR tests take 1-2 days to deliver results to a patient, and rapid antigen tests have limited availability, these dogs could be a valuable asset in preventing further spread of the virus. No more waiting with bated breath for results or wondering whether someone on the same flight caught the virus since their test. This raises the question: if K9s are a common fixture on police forces, why aren’t they working regularly with our medical teams?
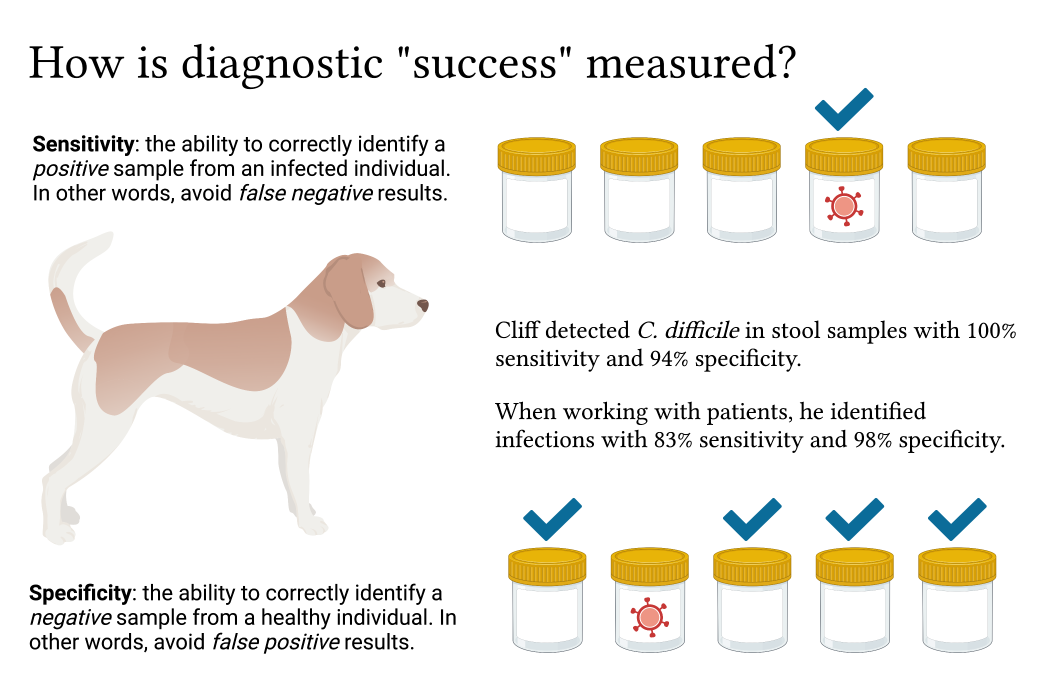
As with all preliminary scientific findings, there is still a need for large-scale, reproducible studies before researchers make broad claims regarding the usefulness of dogs in diagnostics work. The concerns around deploying biomedical detection dogs for COVID-19 testing indicate that dogs may be working with too few samples, or that there is a lot of variability in the success between individual trained dogs. In many previous studies for the detection and diagnosis of infection or disease, the goal was to provide a “proof of principle”, or show that dogs can identify positive samples, rather than run numerous trials with a variety of dogs and patients. While it’s promising that a beagle named Cliff can identify samples contaminated with a bacterial infection at nearly 100% accuracy, does this mean that every trained dog can do the same? Spoiler alert: sadly, no. Scientists are working hard to increase their sample sizes and understand causes of variability in their studies, which could stem from the handlers, patients, or environment.
However, most of the obstacles to establishing a reliable canine workforce in laboratories and hospitals stem from regulatory challenges–specifically, gaining Food and Drug Administration (FDA) approval of dogs as “medical devices”. Although animals have shown promise in the medical diagnostics field since the early 2000s, the process for getting regulatory approval to deploy them in healthcare settings has been unclear. In their paper in Food and Law Drug Journal, Lawyers Matthew Avery and Makenzi Galvan note that:
because FDA’s regulatory purview covers the manufacture and use of diagnostic devices, animals that perform analogous diagnostic functions should also fall within the scope of FDA’s regulatory authority. Development and commercialization of animal-based diagnostics is likely to be stymied by the uncertainty over how the current regulatory regime for diagnostic tests will be applied to animals.
How is a protocol meant for standard medical equipment such as a defibrillator or blood pressure cuff applied to live animals?
Animals inherently have a level of unpredictability beyond that of electrochemical devices and laboratory assays. Scientists running these studies may be in the dark about effects of the handler’s presence on the dogs, and even the identity of the compound that the animals are detecting and signaling for. This may be part of what makes the dogs so good at their job–they can pick up on volatile compounds that scientists haven’t identified or developed an assay for, and they can do it in real time in many different locations and circumstances. However, it also introduces the possibility that animals may introduce false positives or negatives based on factors that scientists or handlers aren’t aware of, such as a secondary odor based on coexisting conditions, diet, or perfume.
Current regulatory guidelines are unable to handle this variability in test outcomes. Although the current evidence suggests that the use of biomedical scent detection dogs may result in efficient, non-invasive, and cost-effective diagnoses for patients, there are no standardized methods for determining the potential risks of misdiagnoses, which could result in additional unneeded testing or a lack of necessary treatment. Avery and Galvan argue that until this type of method for assessing the efficacy of animal-based diagnostics exists, “there are no guarantees that animal-based diagnostics will increase patient outcomes […].” In other words, because the guidelines for developing and evaluating these types of tests haven’t been written, the FDA is unable to approve them for use. Animals will very rarely, if ever, meet the standards designed to approve medical equipment.

The establishment of a new set of guidelines for the approval of biomedical scent detection dogs requires the FDA to write a document that addresses training methods, evaluation of dogs once trained, and the procedures to submit the animal-based diagnostic test for approval. For example, the US Department of Homeland Security (DHS/FEMA) has issued guidelines for the use of dogs in Search and Rescue, and the US Department of Agriculture (USDA/APHIS) has issued a risk assessment for the use of dogs in conservation work. In particular, Search and Rescue dogs must undergo rigorous testing with their handlers, which includes obedience, independent search, alert behavior, and agility. These dogs must be able to quickly and systematically search an area, take directions when searching an area that the handler cannot access, and reliably alert such that handlers can hear the signal when out of sight. Notably, Search and Rescue dogs originated in the 1800s with the well-known and beloved St. Bernard in the Alps, responsible for rescuing over 2,000 people in the treacherous winter conditions of an alpine pass. Although St. Bernards are no longer used for this purpose, the guidelines for this canine profession have continued to improve and expanded to include familiar working breeds such as the labrador retriever, golden retriever, German shepherd, Belgian malinois, and border collie. In comparison to Search and Rescue, biomedical scent detection is still in its infancy.
Biomedical scent detection dogs would require this type of specific training regimen and evaluation for approval to work as part of a medical team. Even without an FDA guidance document, scientists continue to work toward developing their own set of standardized approaches to researching and deploying biomedical scent detection dogs for routine screenings and future pandemics. In Disaster Medicine and Public Health Preparedness, lead author Cynthia M. Otto and colleagues point out the particular advantages to using scent detection dogs for diagnostic testing in the first stages of a pandemic, when a “flexible and rapidly deployable disease screening and testing response” is a necessity for preventing uncontrolled spread. The authors have compiled a list of best practices for biomedical scent detection training, such as the use of “samples obtained from a diversity of people with varying ethnicity, age, gender, concurrent illness that represent the population”, “negative samples from individuals with symptomology similar to the disease in question” such as the common cold or flu, and positive samples from mild and asymptomatic cases.
The authors also outline action items for the future of the biomedical scent detection field, including research support, establishment of standard training procedures and locations, and evidence of beneficial outcomes for the use of dogs in healthcare settings. They conclude that “more research is needed as well as government and community investment into the infrastructure to implement and monitor the effectiveness of this approach.” This final claim gets at the heart of the regulatory issue that scientists face when trying to gain approval for the use of dogs as medical devices–the government and community must buy in and support the use of working dogs in this context. To achieve an FDA guidance document, community members can submit topics for guidance development or pre-written drafts of a suggested guidance. The FDA centers will then determine whether a guidance will be further developed, at which point a selected guidance will be drafted by a special working group, finalized, and issued. In this way, invested community members may work together with the necessary government agencies to progress the establishment of animal-based diagnostic tools such as biomedical scent detection dogs by scientists and healthcare workers.
Scientists are already at the forefront of scent training and animal-based diagnostics–with an FDA guidance document in hand, dogs would be free to enter the healthcare workforce. It may require many more years in the making, but the odds of encountering a working biomedical scent detection dog in a laboratory, hospital, or airport are creeping up. Although we’re all eager to believe that there will be no “next pandemic”, it looks like we’ll be more prepared with canine companions by the sides of healthcare professionals in the future. As the first animals to join the ranks of human society, dogs just keep finding new ways to go above and beyond keeping their end of the deal. As the popular saying goes, “we don’t deserve dogs,” but we sure are lucky to have such good dogs keeping us company.
Support JSTOR Daily! Join our new membership program on Patreon today.